What is Pain Management?
The term pain management refers to the process of reducing chronic or acute pain. Though we have all experienced some sort of physical pain in our lives, getting treatment for pain can often be difficult. Because there are so many types of pain and because tolerance levels vary between individuals, ailments are often misunderstood and ineffectively treated. Pain management is not a “one-size-fits-all” field of medicine, and each patient requires individualized treatment.
Types of Pain
The main two types of pain are acute pain and chronic pain. Acute pain refers to pain that starts suddenly and lasts a short amount of time, whether that’s minutes, hours, or a few days. This type of pain is marked by specific injuries such as broken bones, burns, or cuts that can be traced back to their cause such as getting in a car accident or falling. Other causes of acute pain are dental work, childbirth, and surgery.
Chronic pain, on the other hand, lasts for substantial amounts of time and is experienced daily. Chronic pain can start as acute pain, but the difference is that chronic pain continues long after acute pain should have ended. An example is being in pain a year after a surgery where the expected recovery time was six weeks. Diseases and conditions such as arthritis, cancer, diabetes, and fibromyalgia can contribute to chronic pain.
Other types of pain include bone pain, nerve pain, soft tissue pain, breakthrough pain (sudden increases in pain for patients currently on medication for chronic pain), phantom pain (discomfort in body parts that are no longer there), and referred pain (pain in a location that is different from the cause – such as a heart attack causing pain in the neck or left shoulder).
How to Diagnose and Treat Pain
Because bones, muscles, and nerves all work together in an interconnected system, pain management requires a multi-disciplinary approach to treating different types of pain. Pain management doctors are specialists who recognize the complex nature of pain and understand that pain looks and feels different for every patient.
According to the American Board of Medical Specialties, pain management doctors should be an MD and have board certification for anesthesiology, physical rehabilitation, or psychiatry and neurology. Some clinics also have psychiatrists on staff to help patients deal with the emotional toll that acute or chronic takes.
Much like the human body is interconnected, the goals of pain management go together as well. Because eliminating pain entirely is nearly impossible, the main goal of pain management is to minimize pain. Secondary goals include improving function and increasing the quality of life.
New patients are thoroughly evaluated and have diagnostic tests performed on them. These tests can include X-rays, bloodwork, CT scans, MRI’s, and ultrasounds that doctors use to identify the source of pain. Once doctors come to a diagnosis, they perform treatments, which vary from patient to patient.
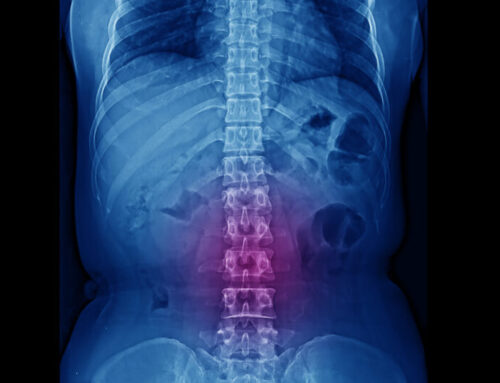
Interventional treatments such as injections or spinal cord stimulation are invasive procedures that deliver medicine directly to the site of pain. With injections, doctors disperse medicine directly to nerve roots, joints, or epidural space, the area between the spinal cord and vertebrae. Relief tends to last longer with direct injections, and doctors evaluate whether or not the specific medication relieves pain. Spinal cord stimulation prevents certain nerves from transmitting pain signals to the brain by sending electrical pulses to those specific nerves. The idea behind this procedure is that pain is masked.
Other forms of treatment include surgery, physical therapy to increase the range of motion, opioids, and other forms of medication. The pain management ladder developed in 1986 is a three-step ladder that shows a progression of treatment that saves strong opioids for last due to their risk of addition. It begins with drug-free treatments, moves to treatments that include small doses of medication, and ends with opioids. Like with all aspects of pain management, the ladder and escalation of treatment will vary with every patient.
Myths about Pain Management
Because pain management is a relatively new field of medicine, there are several myths surrounding it. Don’t fall prey to these myths that may prevent you from seeking the medical care you need!
MYTH: Minor pain doesn’t need to be seen by a physician.
TRUTH: You know your body and what is normal and what isn’t normal. Living with acute or chronic pain for any amount of time can have serious physical and mental effects on everyday life, so reach out to your doctor with any concerns of pain.
MYTH: There is a “silver bullet” for every type of pain.
TRUTH: Unfortunately, there is rarely one solution for chronic or acute pain, and treatments include a combination of interventional treatments, physical therapy, and medication.
MYTH: All doctors are qualified to treat pain.
TRUTH: While all doctors may have a general understanding of what causes chronic and acute pain, it takes years of specialized training and to effectively diagnose and treat pain. It’s important to set yourself up for success when getting pain treatment, and the best way to ensure this is by visiting specialized clinics. Your primary care physician can often refer you to local pain management clinics.
Advanced Pain Institute of Texas is committed to providing world-class pain care in an encouraging and education environment. Dr. Eric Anderson and Dr. John Broadnax work to inspire hope and restore health through cutting-edge, minimally invasive care. Call us today to set up an appointment and reclaim your life from pain!
Share this article
Follow us
A quick overview of the topics covered in this article.